This site is supported by our readers. We may earn a commission, at no cost to you, if you purchase through links.

Medical conditions like eczema and psoriasis also trigger dryness. Overwashing removes protective oils, while indoor heating creates moisture-stealing environments.
Some medications and genetic factors make you more prone to dry skin. Even stress can worsen the condition by affecting your skin’s barrier function.
Think of your skin like a sponge – without proper moisture, it cracks and peels. Understanding these triggers helps you identify which ones might be sabotaging your skin’s health.
Table Of Contents
- Key Takeaways
- Dry Skin Causes
- What Causes Dry Flaky Skin
- Dry Skin Risk Factors
- Skin Conditions and Symptoms
- Dry Skin Clinical Features
- Diagnosing Dry Skin Type
- Treating and Preventing Dry Skin
- Managing Dry Skin Long Term
- Frequently Asked Questions (FAQs)
- Why is my skin flaky over time?
- What causes dry skin?
- What causes dry and flaky skin?
- Is dry flaky skin a symptom of a chronic condition?
- What causes dry skin in older adults?
- Why is my skin drier over time?
- Can diet affect dry skin conditions?
- How often should I moisturize daily?
- When should I see a dermatologist?
- Are there seasonal skincare routine changes?
- Conclusion
Key Takeaways
- Your skin’s aging reduces oil production – After 40, sebum production naturally slows, weakening your protective barrier and making moisture loss inevitable
- Environmental factors strip moisture daily – Hot showers, harsh soaps, cold weather, and low humidity work together to damage your skin’s natural defenses
- Medical conditions accelerate dryness – Eczema, psoriasis, thyroid disorders, and diabetes disrupt your skin barrier, requiring targeted treatment beyond basic moisturizing
- Genetic factors determine your vulnerability – Inherited traits like filaggrin gene mutations make you up to 10 times more prone to chronic dry skin conditions
Dry Skin Causes
You might notice your skin gets dry and flaky from aging, harsh soaps, or changes in weather.
These factors reduce natural oils and damage the skin barrier, making it harder for your skin to stay smooth and comfortable.
They contribute to an overall deterioration of skin health.
Aging and Skin Oil Production
As you age, your skin’s oil factory—sebum production—slows down.
Sebum decline means less moisture and protection. Collagen loss and epidermal thinning weaken your barrier function, making it easier for dryness to sneak in.
Cellular turnover drops, so dead skin lingers.
Decreased natural oil production also occurs after age 40.
Aging and dry skin go hand-in-hand, since skin lipids and natural skin oils fade over time, affecting the skin’s oil factory and leading to dryness.
Environmental Factors and Dryness
Your skin faces a daily battle against environmental factors that strip away its natural moisture.
Cold weather and low humidity create the perfect storm for winter dry skin, while indoor heating systems blow hot, dry air that accelerates moisture loss.
- Cold weather constricts blood vessels, reducing oil production
- Low humidity pulls moisture directly from your skin’s surface
- Sun exposure damages protective barriers and accelerates aging
- Air pollution introduces irritants that inflame and dry skin
These environmental factors work together, making your skin vulnerable to dryness and flaking year-round.
Harsh Soaps and Skin Barrier Damage
Your favorite bar soap might be sabotaging your skin’s natural defenses.
Harsh soap ingredients strip away protective oils, disrupting your skin’s pH balance and barrier function.
These cleansing habits damage the moisture barrier, leaving skin vulnerable to dryness and flaking.
Smart product selection means choosing gentle, pH-balanced cleansers that preserve your skin’s protective layer instead of destroying it, which is crucial for maintaining healthy skin and its natural defenses.
What Causes Dry Flaky Skin
Your skin becomes dry and flaky when its protective barrier breaks down, allowing moisture to escape faster than it can be replaced.
When your skin barrier fails, moisture vanishes faster than you can replace it.
Common triggers include hot showers, harsh soaps, cold weather, aging, and underlying conditions like eczema or thyroid disorders.
Benefits Of Daily Exercise
While understanding dry skin causes helps you recognize triggers, taking care of your overall health can substantially impact your skin’s condition.
Regular physical activity offers surprising benefits for skin health through improved circulation and reduced inflammation.
Here’s how daily exercise supports healthier skin:
- Enhanced Blood Flow – Exercise increases circulation by 17-25%, delivering oxygen and nutrients to skin cells while removing toxins that contribute to dryness.
- Stress Reduction – Physical activity reduces cortisol levels by 26%, preventing stress-related skin barrier damage that leads to moisture loss.
- Better Sleep Quality – Regular movement improves sleep duration in 67% of exercisers, allowing skin to repair and regenerate overnight.
Daily exercise supports Mental Wellbeing, Cardiovascular Health, Weight Management, Energy Levels, and Improved Sleep – all factors that influence skin dryness factors.
When your body functions optimally, your skin care routine becomes more effective at addressing flaky skin reasons and maintaining proper skin health.
Barriers To Healthy Habits
Time constraints plague busy lives, making proper skincare routines feel impossible.
Financial limitations prevent purchasing quality moisturizers that combat dry skin causes.
Knowledge deficit leaves you guessing about flaky skin reasons and skin dryness factors.
Motivation lacking strikes when results take weeks to appear, and accessibility issues mean specialty products remain out of reach.
Environmental skin dryness and harsh soaps continue damaging your skin barrier daily, due to harsh soaps.
Community Wellness Initiatives
While overcoming personal barriers matters, your community offers powerful resources to combat dry skin and flaky skin conditions.
Local wellness programs often provide xerosis education and skin barrier protection workshops that you mightn’t know exist. Incorporating products with ceramides helps repair the skin barrier.
Here are five community initiatives that support skin hydration:
- Public Health clinics offering free dermatology screenings
- Community Education workshops on proper skincare routines
- Support Groups for chronic skin conditions like eczema
- Local Resources providing affordable moisturizers and treatments
- Wellness Programs teaching environmental protection strategies
Dry Skin Risk Factors
While many people know about obvious triggers like harsh soaps and hot showers, certain risk factors for dry skin often go unnoticed.
Your genetics, underlying medical conditions, and even the allergens in your environment can substantially impact your skin’s ability to retain moisture, which is influenced by factors such as genetics.
Medical Conditions and Dry Skin
Medical conditions can wreak havoc on your skin’s moisture levels.
Hypothyroidism effects include rough, scaly patches in 74% of patients.
Diabetes link shows 40-60% experience chronic dryness from increased water loss.
Kidney disease affects half of dialysis patients with xerosis.
Cancer treatments cause widespread flaking in 30-40% of cases, while HIV impact includes markedly dry skin in 60% of patients.
Genetic and Autoimmune Factors
Your genes play a bigger role in dry skin than you might think. If your parents dealt with scaly patches, you’re likely to face similar challenges due to inherited traits.
Key genetic and autoimmune factors include:
- Filaggrin gene mutations – Found in 10-20% of people with chronic eczema and skin barrier damage
- Ichthyosis genetics – Inherited conditions causing fish-scale-like skin texture and severe dryness
- Autoimmune dryness – Conditions like Sjögren’s syndrome reducing natural moisture production substantially
- Psoriasis triggers – Genetic predisposition combined with inflammatory conditions creating persistent scaly plaques
- Genetic mutations – Defective barrier proteins increasing water loss up to 10-fold compared to normal skin
These inherited factors affect your skin’s ability to retain moisture and repair itself properly. Some individuals may also experience inherited ichthyosis types.
Environmental Allergens and Skin Irritation
Around your home, invisible allergens like dust mites, pollen, and pet dander trigger skin sensitivity through direct contact.
These allergen exposures activate your immune response, creating an inflammation cascade that weakens your skin barrier.
Your body’s allergic dermatitis develops when repeated allergen exposure causes skin reactions, and practicing allergen avoidance helps prevent skin allergies.
This approach reduces irritating skin irritants, and by understanding the role of skin barrier weakening, you can better manage and prevent allergic reactions.
Skin Conditions and Symptoms
Sometimes your skin acts out because of underlying conditions you mightn’t realize you have.
When eczema, psoriasis, or seborrheic dermatitis strike, they create the perfect storm for dry, flaky skin that won’t quit no matter how much lotion you slather on.
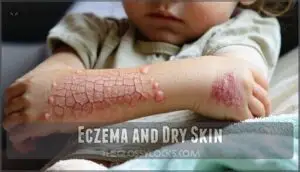
Eczema and Dry Skin
Eczema affects 31 million Americans, creating a frustrating cycle where inflammation damages your skin’s protective barrier.
This leads to moisture loss and makes existing dry skin worse. The condition involves several eczema types, including atopic dermatitis, which causes chronic skin itching and inflammation.
- Your skin feels like sandpaper – rough, cracked patches that never seem to heal
- Sleep becomes impossible – relentless itching keeps you awake at night
- Simple tasks hurt – washing dishes or putting on clothes causes stinging pain
Childhood eczema often starts early, with eczema triggers including harsh soaps, stress, and allergens. Understanding this dry skin overlap helps with effective eczema management through proper moisturizing and avoiding irritants.
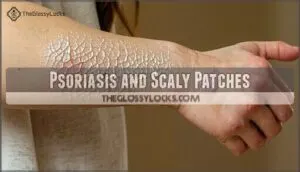
Psoriasis and Scaly Patches
Psoriasis triggers an autoimmune response that accelerates skin cell production, creating thick scaly skin patches faster than your body can shed them.
This chronic skin inflammation affects over 7.5 million Americans, producing raised plaques with silvery scales.
You’ll notice these distinctive skin scales on elbows, knees, and scalp psoriasis areas, while some experience nail psoriasis or psoriatic arthritis complications.
Seborrheic Dermatitis and Greasy Scalp
Unlike ordinary dry skin, seborrheic dermatitis creates a paradox where your scalp produces excess oil yet develops flaky, crusty scales.
This skin condition involves yeast overgrowth that triggers scalp inflammation, making treatment options essential for managing symptoms.
Key characteristics include:
- Greasy yellow scales – Unlike regular dandruff severity, these oily flakes stick to your scalp and hair
- Cradle cap in infants – The childhood version creates thick, crusty patches on baby scalps
- Chronic scalp itchiness – Persistent irritation that worsens with stress and cold weather
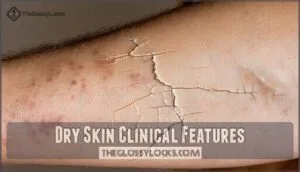
Dry Skin Clinical Features
When you have dry, flaky skin, you’ll notice your skin feels rough and may crack, especially when the dryness becomes severe.
You might also experience itching, pain, peeling, and stinging sensations that make daily activities uncomfortable.
Rough Skin Texture and Cracking
When your skin loses its natural moisture, you’ll notice its surface becomes rough like sandpaper.
This skin roughness creates an uneven texture that feels bumpy to touch.
Deep skin fissures can develop as skin dryness worsens, creating painful cracks that pose a bleeding risk.
These breaks in your skin barrier also increase infection risk.
Proper texture improvement requires addressing underlying skin cracking patterns and managing associated pain effectively.
Itchiness and Associated Pain
That familiar itch can quickly turn from mild annoyance to relentless torment.
Don’t let that innocent itch become your skin’s worst enemy.
Scratching complications arise when you can’t resist the urge, creating wounds that invite infection.
This skin discomfort disrupts sleep cycles, leaving you exhausted and irritable.
Inflammation triggers nerve endings, amplifying skin pain beyond the original irritation, which can significantly impact your quality of life.
Constant skin irritation mounts from constant skin irritation, as psychological impact suffers.
Peeling and Stinging Sensations
Beyond surface irritation, your skin might experience deeper discomfort as Severity Factors worsen.
Peeling reveals raw layers underneath, while stinging creates sharp skin pain that signals barrier damage.
These Sensation Triggers affect different skin areas uniquely – your face burns differently than your hands.
Effective Symptom Management requires identifying specific Relief Methods, whether cool compresses reduce skin burning or gentle moisturizers ease skin discomfort and persistent itching.
Diagnosing Dry Skin Type
Getting the right diagnosis matters because what looks like simple dry skin could actually be eczema, psoriasis, or another condition requiring different treatment.
Your doctor will examine your skin closely and may order tests to rule out underlying medical causes like thyroid problems or diabetes.
Physical Examination and Medical History
When your doctor evaluates dry skin, they’ll conduct a thorough skin examination and review your medical history.
They’ll ask about symptom onset, current medications, and family medical history of skin conditions. This medication review helps identify potential triggers, while evaluating comorbidities like diabetes or thyroid disorders.
Your family history reveals genetic predispositions to conditions causing persistent dryness. Additionally, a family history of eczema may point to genetic predispositions that exacerbate dryness.
Skin Biopsy and Laboratory Tests
When standard examination isn’t enough, your doctor might recommend advanced biopsy techniques and lab analysis for diagnostic accuracy.
A skin biopsy reveals microscopic tissue changes, distinguishing between eczema, psoriasis, and other skin conditions through detailed skin examination.
Laboratory tests check thyroid function, vitamin levels, and immune markers. However, test limitations exist—results need careful interpretation alongside your symptoms for proper diagnosis, considering the need for careful interpretation.
Differential Diagnosis and Ruling Out Conditions
Your doctor plays detective, separating true dry skin from tricky mimickers.
Eczema vs. dryness requires examining inflammation patterns and family history.
Psoriasis mimics often show thick, silvery scales versus simple flaking.
Different dermatitis types need specific treatments.
Ichthyosis screening checks for genetic markers.
Systemic mimickers like thyroid disorders require blood tests to rule out underlying causes affecting your skin diagnosis.
Treating and Preventing Dry Skin
Now that you know what causes dry flaky skin, you can take steps to treat and prevent it.
The right moisturizers, simple lifestyle changes, and avoiding harsh products can restore your skin’s natural barrier and keep it healthy.
Moisturizers and Topical Treatments
You’ll need the right moisturizers to repair your skin’s protective barrier.
Look for products containing ceramides, hyaluronic acid, and glycerin – these humectant types draw moisture into your skin.
Emollient benefits come from ingredients like shea butter that smooth roughness.
Occlusive agents like petrolatum lock in hydration.
Many individuals find relief using ceramide-based formulations.
OTC treatments work well, but prescription creams may be necessary for severe cases.
Lifestyle Measures and Home Remedies
Simple home remedies work wonders for dry skin triggers.
Oatmeal baths soothe irritation while natural oils lock in moisture.
Gentle exfoliation removes dead cells without damage.
Hydration importance can’t be overstated—drink plenty of water daily.
Humidifier benefits include raising indoor moisture levels by 21%.
Oatmeal bath products can further alleviate irritation.
These skin care tips complement your moisturizing routine effectively, and hydration is key to maintaining healthy skin.
Avoiding Harsh Soaps and Extreme Temperatures
Your daily bathing habits can make or break your skin’s health.
Hot showers and harsh soap ingredients strip away natural oils that protect against dry skin triggers. Keep water temperature lukewarm and choose gentle, fragrance-free cleansers.
Cold temperatures demand extra winter skincare protection—use humidifiers indoors and apply sun protection year-round for ideal skin care tips.
Managing Dry Skin Long Term
Once you understand what triggers your dry, flaky skin, you’ll need a solid plan to keep it healthy over time.
Managing chronic dry skin means working closely with healthcare providers and staying consistent with your skincare routine.
Working With Healthcare Providers
Your healthcare provider becomes your ally in conquering stubborn dry skin.
Schedule regular check-ups to discuss Treatment Adherence and monitor progress.
A dermatologist can provide Specialist Referrals when needed and adjust Medication Management strategies.
Clear Doctor Communication helps identify triggers you might miss.
Your skin care provider develops personalized Preventative Strategies, ensuring medical care evolves with your changing needs.
Monitoring Skin Condition and Adjusting Treatment
Your skin’s response to Treatment Efficacy varies over time, making regular Symptom Tracking essential for success.
Monitor changes weekly, noting how your skin reacts to different skin care products and Environmental Impact factors like humidity levels.
Document what triggers flare-ups during Seasonal Changes. Make Routine Adjustments based on these observations – your skin condition management strategy isn’t set in stone.
Maintaining a Healthy Skin Care Routine
Establishing consistent habits becomes your foundation for managing dry, flaky skin effectively.
Your skin care routine should focus on gentle cleansing and hydration importance while protecting against environmental damage. Many find relief using products without fragrance.
- Gentle Cleansing: Use lukewarm water and mild, fragrance-free cleansers that won’t strip natural oils
- Hydration Importance: Apply moisturizer immediately after bathing to lock in moisture and maintain skin hydration
- Sun Protection: Use broad-spectrum SPF daily to prevent UV damage and premature aging
- Exfoliation Frequency: Limit skin exfoliation to once weekly with gentle products containing appropriate product ingredients
Frequently Asked Questions (FAQs)
Why is my skin flaky over time?
Like an old-fashioned washboard worn smooth, your skin’s natural oil production decreases with age.
Environmental factors, harsh soaps, and hot showers strip away moisture, leaving your skin barrier compromised and flaky over time.
What causes dry skin?
Your skin gets dry when it loses moisture faster than it can replace it.
This happens due to aging, harsh soaps, hot showers, cold weather, medical conditions, or genetics affecting your skin’s natural barrier.
What causes dry and flaky skin?
Aging, harsh soaps, hot showers, cold weather, and low humidity strip your skin’s natural oils. Medical conditions like eczema, psoriasis, hypothyroidism, and diabetes also contribute to persistent dryness and flaking.
Is dry flaky skin a symptom of a chronic condition?
Persistent patches point to possible problems.
Yes, you’ll find dry flaky skin often signals chronic conditions like eczema, psoriasis, hypothyroidism, or diabetes.
These underlying issues disrupt your skin’s natural barrier function, creating ongoing dryness that needs medical attention, often related to chronic conditions.
What causes dry skin in older adults?
As you age, your skin produces less oil and loses moisture more easily.
Cold weather, hot showers, harsh soaps, and medications like diuretics worsen dryness by stripping your skin’s protective barrier.
Why is my skin drier over time?
Your skin gets drier as you age because your oil glands produce less sebum after Environmental factors like heating, hot showers, and harsh soaps also strip away natural moisture.
Can diet affect dry skin conditions?
Yes, your diet can substantially impact dry skin conditions.
Poor nutrition, especially deficiencies in essential fatty acids, vitamins A, D, and E, can worsen skin dryness and slow healing of flaky patches.
How often should I moisturize daily?
Apply moisturizer twice daily—morning and evening—to lock in hydration. After bathing, when your skin’s still damp, it’s the perfect time to seal in moisture effectively.
When should I see a dermatologist?
See a dermatologist if symptoms persist despite moisturizing, worsen rapidly, show signs of infection, or include severe itching, bleeding, or unusual changes in appearance.
Are there seasonal skincare routine changes?
Winter drops humidity by 50%, dramatically affecting your skin’s moisture barrier. You’ll need heavier moisturizers, gentle cleansers, and humidifiers during cold months, while summer requires lighter products and increased sun protection.
Conclusion
Understanding what causes dry flaky skin transforms your skincare approach like a gardener learning why plants wither.
Armed with knowledge about aging, harsh soaps, environmental factors, and medical conditions, you’re equipped to protect your skin‘s natural barrier.
Remember that addressing what causes dry flaky skin requires patience and consistency.
Don’t let hidden triggers sabotage your skin’s health—take control today and restore your skin’s natural moisture balance.